Contents
Introduction
This article focuses on clinically relevant aspects of tic disorders.
What are "Tics"
Hallmark of tic disorders are involuntary/semivoluntary, sudden, rapid, recurrent, unpredictable, non-rhythmic movements (motor tics) and sounds (vocal tics). Distinguishing tics from other hyperkinetic movement phenomena can be tricky; the following characteristics of tics are useful in making accurate diagnosis:
- irregularity of tics distinguish them from tremors
- waxing and waning pattern as well as worsening with stress and excitement can help distinguished tics from compulsions and stereotypies.
- Motor and vocal tics are often preceded by premonitory urges
- Patients are generally able to briefly suppress onset of tics, but the premonitory tension or discomfort/anxiety rises
- Once an episode of tics occur, there is a brief feeling of relief
- Stress, fatigue, and even excitement can exacerbate tics
Consider in the differential diagnosis: stereotypies of autism spectrum disorders, chorea, athetosis, myoclonus, dystonia, paroxysmal dyskinesias, compulsions of OCD, seizures, and, of course, “pseudoseizures,” restless legg syndrome.
Tics can be simple or complex:
Simple tics involve only one motor group.
| Simple Tics | Complex Tics | |
| Motor Tics | Eye blinking, sticking tongue out, head jerking |
Coordinated patterns of sequential movements: touching the nose, echopraxia, copropraxia, smelling objects, kissing self, others, arm flapping |
| Vocal Tics | Barking, yelling, throat clearing | Coprolalia, echolalia, palilalia |
Epidemiology
- Prevalence of tic disorders (transient or chronic) can b as high as is 19% in school-age children; Tourette's syndrome is present in 0.1%-3.6% of youth.
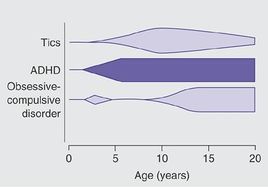
- There is 2:1 M:F predominance; peak onset of chronic tic disorders in 7 years of age. Peak symptom severity is 9-12 y.o.
- Tics associated with Tourette's disorder peak before puberty and begin to subside after age 12.
- OCD associated with Tourette's disorder tends to occur around age 12-14, earlier than OCD in children without tics.
- Comorbidites are the rule rather than an exception, particularly ADHD, OCD, learning, and sleep disorders.
- while there is a warning about use of stimulants to treat ADHD in children with tics, it is not based on any large studies. In practice, tics may increase transiently in as many as 20% of children put on a stimulant. (Blooch 2009). Since morbidity/disability of ADHD is very significant, it is important to treat.
Prognosis
- About 25% of youth with tics will continue to have tics as adults.(1)
DSM diagnosis
While tics can be primary (idiopathic or inherited) or secondary (due to drugs, infection, or developmental disorders), the DSM-IV classified tics by other characteristics:
- Tourette Syndrome involves frequent motor AND vocal tics (must have both, but not necessarily concurrently), starting before age of 18 and lasting for 1 year
- If frequent vocal OR motor tics start before 18 and last for a year, the diagnosis is Persistent (Chronic) motor or vocal tic disorder
DSM-5 changes
- Tic disorders are now categorized under Neurodevelopmental disorders.
- Transient tic disorder had been renamed to Provisional tic disorder, which include all tics present less than 1 year.
Diagnostic Pearls
- Unlike other movement disorders, tics can occur during sleep.
- Document family history of tics when evaluating a child
- Order TSH: thyroid dysfunction is a frequent comoridity
- Sudden onset or worsening of symptoms: obtain Group A beta-hemolytic strep swab, ASO titer, and anti-DNAse B leves (think PANDAS)
- Rule out other secondary causes: head trauma, stroke, autism, CO poisoning, hypoglycemia
- Rule out drugs and intoxication as potential causes: antidepressants, anticholinergics, antihistamines, levodopa, antiepileptics
Treatment
- Behavioral and supportive treatments include psychoeducation, sleep hygeine, physical exercise, emotional support
- Habit reversal training HRT is a behavioral therapy centered on interruption of stimulus-response sequences was shown to be effective in RCTs
- HRT involves 1) awareness training and 2) competing response practice.
- Pharmocological treatments
- Dopamine-R antagonists: pimozide (most effective, but requires EKG monitoring for arrhythmias and most EPS-inducing) and haloperidol have the strongest evidence.
- Next in line chlorpromazine, fluphenazine, risperdone (may be best tolerated)
- Alpha-adrenergics can ameliorate both tics and comorbid ADHD with milder side effects: clonidine, guanfacine are safe and effective (Level of evidence B)
- Dopamine-R agonists, at low doses (pergolide), benzodiazepines (clonazepam), and calcium-channel blockers (not diltiazem) may have a role;
- SSRIs are used for comorbid OCD
- Other treatments including botox (B), tiapride, nicotine patch, topiramate (B), donepezil, cannabinoids, DBS have been used.
High-yield facts
Tics
- Coprolalia/copropraxia = obscene words and gestures are complex vocal and motor tics
- Echolalia/echopraxia = mimicking other’s sounds and gestures are considered complex tics
- Jerks that last less than 200 ms are most likely myoclonus (not tics)
- Cannabis, alcohol, and nicotine may decrease tics
- Stimulants, stress, fatigue, heat exposure, caffeine, dopamine agonists, and beta-hemolytic strep infection can exacerbate tics
Tourette syndrome
- to diagnose TS, need 2 or more motor tics and at least 1 vocal tic at some time during the illness
- onset typically before age of 7
- symptoms typically peak around 9-11 years of age, and subside in adolescence
- less than 10% fully recover
- Common comorbidities include OCD and ADHD
- M:F ratio is 5:1
Further Reading
1. Murphy TK, et. al. Practice Parameter for the Assessment and Treatment of Children and Adolescents With Tic Disorders JAACAP 2013;52(12):1341–1359
Facts for Families from AACAP website. Updated in 2004;
Prescribing Psychotropic Medications to Children Practice parameters from AACAP. Updated 2009
Tourette Syndrome Association has medical articles, family information, and videos on TS
|
Article Progress | |||||||||
| Write | Edit | Finalize | |||||||
Content |
Completeness | Index Links | Trial Release | Final Check | |||||
.